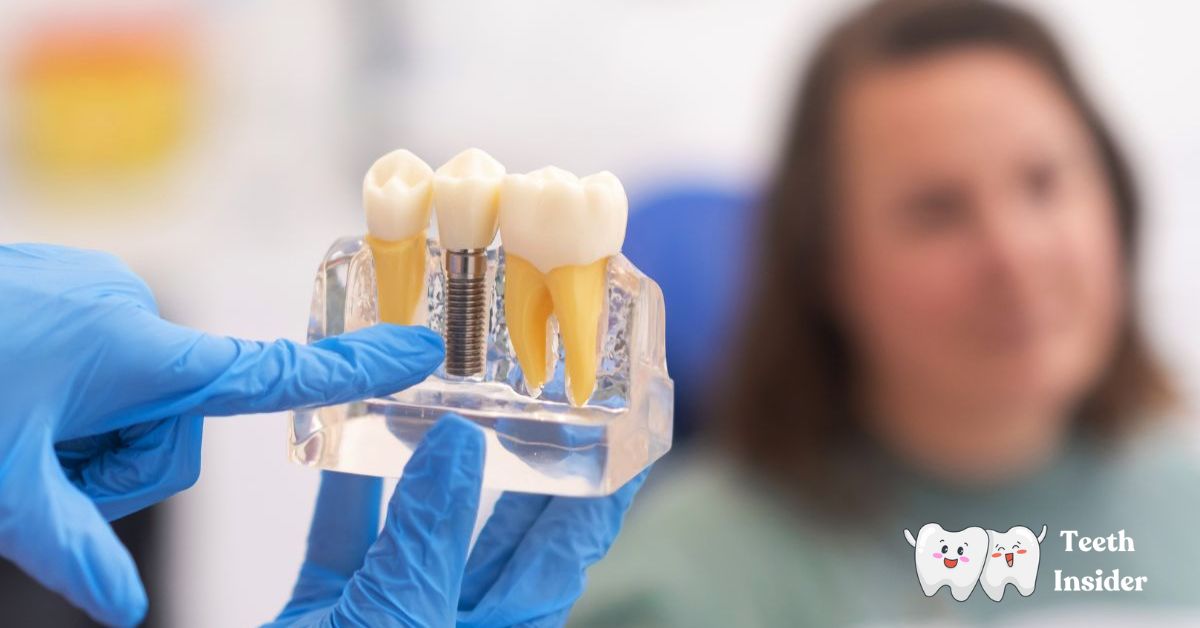
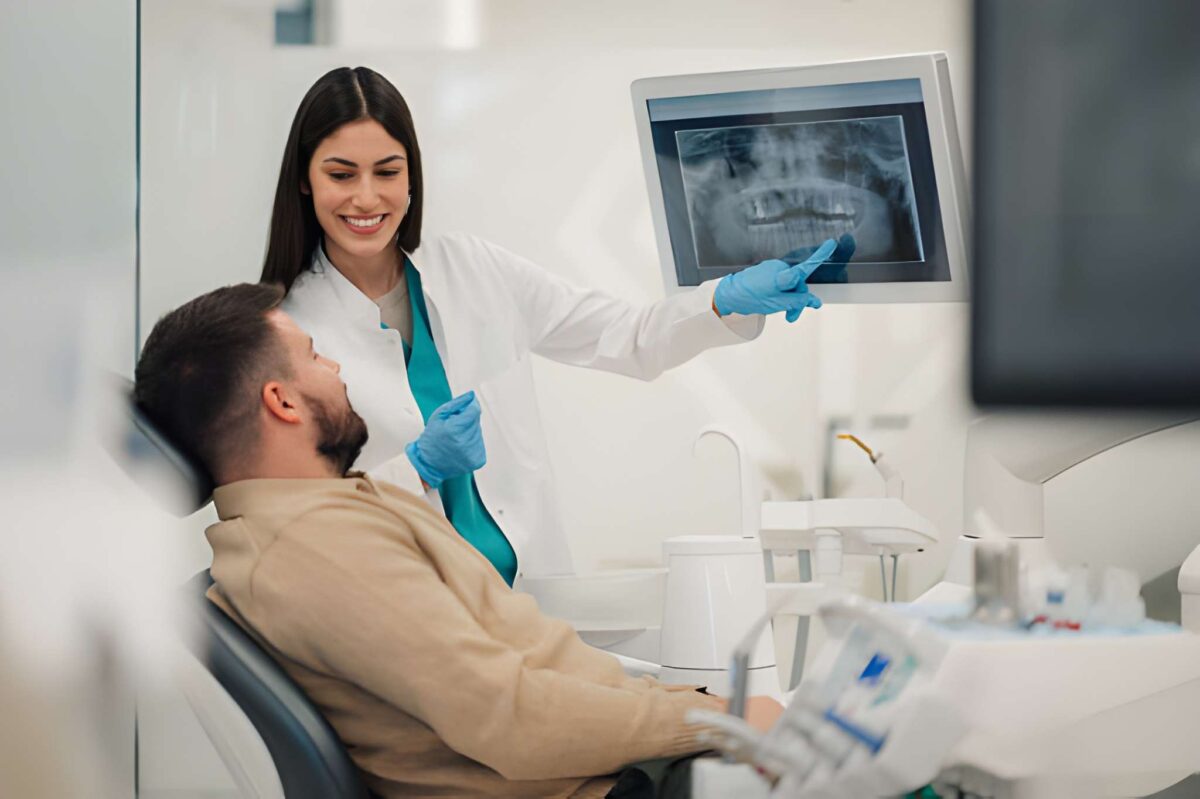
NHS dentistry works by providing clinically necessary dental care through practices funded under fixed NHS contracts.
Access, treatment availability, and recall intervals depend on funding limits, clinical need, and local capacity rather than permanent patient registration.
Introduction
Many people assume NHS dentistry works like GP services. It does not. Dental care under the NHS follows a different funding and access model, which explains why availability varies, why recall intervals differ, and why some practices stop taking new patients.
How NHS Dentistry Works in Practice
NHS dental practices operate under annual NHS contracts.
These contracts:
- Set how much NHS treatment a practice can provide
- Limit the number of funded appointments
- Prioritise treatment based on clinical need
Once a practice reaches its NHS allocation, it may stop accepting new NHS dental patients until funding resets.
What NHS Dental Care Covers
NHS dentistry focuses on essential oral health, not cosmetic outcomes.
It typically includes:
- Dental examinations
- X-rays where clinically required
- Fillings and extractions
- Root canal treatment (where appropriate)
- Dentures and bridges
Treatments are provided only when there is a clear clinical need.
How NHS Dental Charges Work
NHS dental charges are banded nationally in England.
Each band covers:
- A defined group of treatments
- All necessary care within that band
Patients pay one charge per course of treatment, not per visit.
Registration and Access
There is no permanent NHS dental registration.
Instead:
- Patients remain on a practice list while attending
- Long gaps may result in removal
- Practices can close lists when funding is used
This is why guidance on How to get an NHS dentist is often needed.
Recall Intervals and Appointments
Check-up frequency is based on risk, not habit.
Dentists may recommend:
- Short recall intervals for higher-risk patients
- Longer intervals for patients with stable oral health
This approach allows resources to be focused where care is most needed.
Emergency and Urgent NHS Dental Care
Even without routine access, NHS dentistry still provides:
- Emergency pain relief
- Treatment for infection or trauma
Urgent care does not register a patient permanently with a practice.
Why Availability Varies by Location
Access differs because:
- NHS funding is capped
- Dentist workforce levels vary
- Demand differs between regions
Some areas have better access simply due to contract distribution.
Common Misunderstandings
- NHS dentists are not private dentists offering NHS discounts
- Being treated once does not guarantee ongoing access
- Practices are limited by funding, not willingness
Understanding these limits helps manage expectations.
FAQs
Is NHS dentistry free?
Some patients qualify for free care, but most adults pay set NHS charges.
Can an NHS dentist refuse treatment?
They can refuse non-essential care if funding limits are reached.
Do NHS dentists work privately too?
Many practices offer both NHS and private treatment.
Is cosmetic dentistry covered by the NHS?
No. Cosmetic procedures are not funded.
Can I switch NHS dentists?
Yes, if another practice has NHS availability.
Are children treated differently?
Children are prioritised, but access still depends on local capacity.
Does emergency care count as NHS registration?
No. Emergency treatment does not register a patient.
Who oversees NHS dentistry?
The NHS sets national policy and funding frameworks.
Author: Teeth Insider Editorial Team
Last updated: January 2026